Introduction
Osteoarthritis is the most common form of arthritis and is often referred to as “wear and tear” arthritis. It occurs when the protective cartilage that cushions the ends of the bones within a joint gradually wears down over time. This degeneration leads to joint pain, stiffness, and other troublesome symptoms. While osteoarthritis can affect any joint in the body, it most commonly affects the knees, hips, hands, and spine.What is Osteoarthritis?
Definition of Osteoarthritis
Osteoarthritis is a degenerative joint disease characterized by the breakdown of cartilage, the smooth tissue that covers the ends of bones where they meet to form a joint. As the cartilage deteriorates, the bones can rub against each other, causing pain, swelling, and loss of motion in the affected joint.Prevalence and Impact of Osteoarthritis
Osteoarthritis is a widespread condition, particularly among older adults. According to the Arthritis Foundation, over 32.5 million adults in the United States alone are affected by osteoarthritis. It is a leading cause of disability,contributing to decreased quality of life and increased healthcare costs.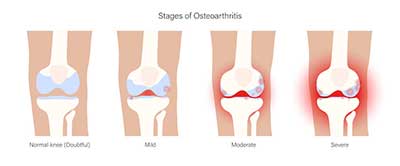
Causes and Risk Factors
Several factors contribute to the development of osteoarthritis. Understanding these causes and risk factors can help individuals take preventive measures and manage the condition effectively.Age and Osteoarthritis
Advancing age is one of the primary risk factors for osteoarthritis. As we grow older, the cartilage in our joints naturally wears down, making them more susceptible to damage and degeneration.Genetics and Osteoarthritis
Genetic factors can also play a role in the development of osteoarthritis. Some people may inherit certain gene variations that affect the structure and stability of their joints, increasing their risk of developing the condition.Obesity and Osteoarthritis
Excess weight puts additional stress on the joints, especially the knees and hips. The increased pressure can accelerate the breakdown of cartilage, leading to the early onset and progression of osteoarthritis.Joint Injuries and Osteoarthritis
Joint injuries, such as fractures or ligament tears, can increase the risk of developing osteoarthritis in the affected joint. Damage to the cartilage and surrounding structures can disrupt the joint’s normal function and lead to the development of the condition.
Common Symptoms of Osteoarthritis
Recognizing the symptoms of osteoarthritis is crucial for early diagnosis and intervention. The following are the most common signs and symptoms experienced by individuals with osteoarthritis.Joint Pain and Stiffness
Pain and stiffness in the joints are hallmark symptoms of osteoarthritis. The pain is typically described as a dull ache that worsens with movement and improves with rest. Morning stiffness is also common, where individuals may experience difficulty moving the affected joint after periods of inactivity.Swelling and Inflammation
Inflamed joints may appear swollen and feel warm to the touch. The inflammation is a result of the body’s immune response to the breakdown of cartilage and the subsequent release of inflammatory mediators.Decreased Range of Motion
As osteoarthritis progresses, the range of motion in the affected joint may become limited. Individuals may find it challenging to fully bend, straighten, or rotate the joint, impacting their ability to perform daily activities.Bone Spurs and Joint Deformities
In some cases, osteoarthritis can lead to the development of bone spurs, also known as osteophytes. These bony projections can cause joint deformities, leading to further pain and functional impairment.
How Osteoarthritis Affects Different Parts of the Body
Osteoarthritis can affect various joints in the body, and its symptoms may vary depending on the location. Let’s explore how osteoarthritis commonly affects different body parts.Osteoarthritis in the Knees
Knee osteoarthritis is one of the most prevalent forms of the condition. It can cause pain, swelling, and stiffness in the knee joint, making it difficult to walk, climb stairs, or engage in physical activities.Osteoarthritis in the Hips
Hip osteoarthritis can result in pain and limited mobility in the hip joint. Individuals may experience discomfort while walking, sitting for prolonged periods, or performing activities that require hip movement.Osteoarthritis in the Hands and Fingers
Osteoarthritis can affect the joints in the hands and fingers, leading to pain, stiffness, and difficulty grasping objects. Swelling and the development of bony nodules at the finger joints are common in this form of osteoarthritis.Osteoarthritis in the Spine
Spinal osteoarthritis primarily affects the facet joints, which are located between the vertebrae in the spine. This can cause back pain, stiffness, and reduced flexibility. In severe cases, spinal osteoarthritis can lead to compression of the nerves, resulting in radiating pain or numbness in the arms or legs.
Diagnosing Osteoarthritis
Diagnosing osteoarthritis involves a combination of medical history, physical examination, and diagnostic tests. While there is no single definitive test for osteoarthritis, healthcare professionals use several methods to assess joint damage and determine the extent of the condition.Physical Examination
During a physical examination, the healthcare provider will assess the affected joint’s range of motion, look for signs of swelling or inflammation, and check for joint tenderness. They may also ask about symptoms, medical history, and any previous injuries.Imaging Tests (X-rays, MRI)
Imaging tests such as X-rays and magnetic resonance imaging (MRI) can provide detailed images of the affected joint. X-rays can reveal joint damage, including cartilage loss, bone spurs, and joint alignment changes. MRIs are particularly useful in assessing soft tissues such as cartilage and ligaments.Joint Fluid Analysis
In some cases, a joint fluid analysis, also known as arthrocentesis, may be performed. This involves removing a small amount of fluid from the affected joint using a needle. The fluid is then analyzed for signs of inflammation, infection, or other conditions.
Treatment Options for Osteoarthritis
While there is no cure for osteoarthritis, various treatment options are available to manage symptoms, improve joint function, and enhance quality of life. The choice of treatment depends on the severity of the condition, the affected joint, and the individual’s overall health.Lifestyle Changes and Self-Care
Making certain lifestyle modifications can help alleviate symptoms and slow the progression of osteoarthritis. These include maintaining a healthy weight to reduce stress on the joints, engaging in regular low-impact exercise, using joint protection techniques, and applying hot or cold packs to alleviate pain and inflammation.Medications for Pain Management
Over-the-counter pain relievers such as acetaminophen and nonsteroidal anti-inflammatory drugs (NSAIDs) can help manage mild to moderate osteoarthritis pain. In some cases, healthcare providers may prescribe stronger pain medications or recommend topical creams or gels for localized relief.Physical Therapy and Exercise
Physical therapy plays a crucial role in managing osteoarthritis. A physical therapist can create a personalized exercise program to improve joint flexibility, strengthen the surrounding muscles, and enhance overall function. They may also use techniques such as heat therapy, electrical stimulation, or manual therapy for pain relief.Assistive Devices and Joint Support
Assistive devices such as braces, splints, or canes can provide support to the affected joint and alleviate pain. In some cases, custom orthotics or shoe inserts may be recommended to improve joint alignment and reduce pressure on specific areas.Surgical Interventions
For severe cases of osteoarthritis that do not respond to conservative treatments, surgical interventions may be considered. These can include joint repair, joint replacement, or joint fusion surgeries, depending on the extent of joint damage and the individual’s overall health.
Coping with Osteoarthritis
Living with osteoarthritis can be challenging, but there are strategies individuals can employ to cope with the condition and minimize its impact on daily life.Pain Management Techniques
In addition to medications, various pain management techniques can help individuals cope with osteoarthritis-related pain. These include applying heat or cold therapy, practicing relaxation techniques such as deep breathing or meditation, and exploring alternative therapies like acupuncture or massage.Support Groups and Counseling
Joining support groups or seeking counseling can provide valuable emotional support for individuals with osteoarthritis. Connecting with others who are going through similar experiences can help alleviate feelings of isolation and provide practical tips for managing the condition.Lifestyle Adjustments
Making necessary adjustments to daily routines and activities can make a significant difference in managing osteoarthritis symptoms. This may involve pacing oneself, taking breaks when needed, and utilizing assistive devices or ergonomic tools to reduce joint strain.
Prevention of Osteoarthritis
While osteoarthritis cannot always be prevented, certain measures can help reduce the risk of developing the condition or slow its progression.Maintaining a Healthy Weight
Maintaining a healthy weight is crucial for joint health. Excess weight puts additional stress on the joints, especially the weight-bearing joints like the knees and hips. By adopting a balanced diet and engaging in regular exercise, individuals can manage their weight and reduce the strain on their joints.Regular Exercise and Stretching
Regular exercise is essential for maintaining joint flexibility, muscle strength, and overall joint health. Low-impact activities such as walking, swimming, or cycling can help strengthen the muscles around the joints and improve their stability. Stretching exercises can also improve joint range of motion and prevent stiffness.Protecting Joints from Injury
Taking precautions to protect the joints from injury can help prevent the development of osteoarthritis. This includes using proper techniques when lifting heavy objects, wearing protective gear during sports or physical activities, and avoiding repetitive motions that put excessive strain on the joints.Managing Other Health Conditions
Certain health conditions, such as diabetes or metabolic disorders, can increase the risk of developing osteoarthritis. By effectively managing these underlying conditions, individuals can minimize the impact on joint health and reduce the likelihood of developing osteoarthritis.The 5 Best Bitcoin Wallets for Safe and Secure Storage
Conclusion
Understanding the symptoms of osteoarthritis is crucial for early detection, intervention, and effective management of the condition. By recognizing the signs such as joint pain, stiffness, and limited mobility, individuals can seek appropriate medical attention and explore various treatment options available. With a combination of lifestyle modifications, pain management strategies, and support, individuals can cope with osteoarthritis and improve their quality of life.Are there any similarities in the symptoms of Anorexia and Osteoarthritis?
Recognizing anorexia signs can be crucial in identifying the disorder early on. However, it is important to note that anorexia and osteoarthritis have distinct symptoms. Anorexia primarily affects one’s eating habits, leading to severe weight loss, while osteoarthritis affects the joints, causing pain, stiffness, and mobility issues. Though both conditions require attention, they differ greatly in terms of symptoms and treatment approaches.
IntroductionWhat is Osteoarthritis?Definition of OsteoarthritisPrevalence and Impact of OsteoarthritisCauses and Risk FactorsAge and OsteoarthritisGenetics and OsteoarthritisObesity and OsteoarthritisJoint Injuries and OsteoarthritisCommon Symptoms of OsteoarthritisJoint Pain and StiffnessSwelling and InflammationDecreased Range of MotionBone Spurs and Joint DeformitiesHow Osteoarthritis Affects Different Parts of the BodyOsteoarthritis in the KneesOsteoarthritis in the HipsOsteoarthritis in the Hands and FingersOsteoarthritis in the SpineDiagnosing OsteoarthritisPhysical ExaminationImaging Tests (X-rays, MRI)Joint Fluid AnalysisTreatment Options for OsteoarthritisLifestyle Changes and Self-CareMedications for Pain ManagementPhysical Therapy and ExerciseAssistive Devices and Joint SupportSurgical InterventionsCoping with OsteoarthritisPain Management TechniquesSupport Groups and CounselingLifestyle AdjustmentsPrevention of OsteoarthritisMaintaining a Healthy WeightRegular Exercise and StretchingProtecting Joints from InjuryManaging Other Health ConditionsConclusionAre there any similarities in the symptoms of Anorexia and Osteoarthritis?FAQs1. Can osteoarthritis be cured completely?2. How can I manage the pain associated with osteoarthritis?3. Are there any natural remedies for osteoarthritis?4. Can osteoarthritis affect young people?5. Is osteoarthritis the same as rheumatoid arthritis?





